Related Research Articles

Type 2 diabetes (T2D), formerly known as adult-onset diabetes, is a form of diabetes mellitus that is characterized by high blood sugar, insulin resistance, and relative lack of insulin. Common symptoms include increased thirst, frequent urination, fatigue and unexplained weight loss. Symptoms may also include increased hunger, having a sensation of pins and needles, and sores (wounds) that do not heal. Often symptoms come on slowly. Long-term complications from high blood sugar include heart disease, stroke, diabetic retinopathy which can result in blindness, kidney failure, and poor blood flow in the limbs which may lead to amputations. The sudden onset of hyperosmolar hyperglycemic state may occur; however, ketoacidosis is uncommon.
In medicine, comorbidity refers to the simultaneous presence of two or more medical conditions in a patient; often co-occurring with a primary condition. It originates from the Latin term morbus prefixed with co- ("together") and suffixed with -ity. Comorbidity includes all additional ailments a patient may experience alongside their primary diagnosis, which can be either physiological or psychological in nature. In the context of mental health, comorbidity frequently refers to the concurrent existence of mental disorders, for example, the co-occurrence of depressive and anxiety disorders. The concept of multimorbidity is related to comorbidity but is different in its definition and approach, focusing on the presence of multiple diseases or conditions in a patient without the need to specify one as primary.

Ambulatory care or outpatient care is medical care provided on an outpatient basis, including diagnosis, observation, consultation, treatment, intervention, and rehabilitation services. This care can include advanced medical technology and procedures even when provided outside of hospitals.

Pain management is an aspect of medicine and health care involving relief of pain in various dimensions, from acute and simple to chronic and challenging. Most physicians and other health professionals provide some pain control in the normal course of their practice, and for the more complex instances of pain, they also call on additional help from a specific medical specialty devoted to pain, which is called pain medicine.

Pharmacogenomics, often abbreviated "PGx," is the study of the role of the genome in drug response. Its name reflects its combining of pharmacology and genomics. Pharmacogenomics analyzes how the genetic makeup of a patient affects their response to drugs. It deals with the influence of acquired and inherited genetic variation on drug response, by correlating DNA mutations with pharmacokinetic, pharmacodynamic, and/or immunogenic endpoints.
Calorie restriction is a dietary regimen that reduces the energy intake from foods and beverages without incurring malnutrition. The possible effect of calorie restriction on body weight management, longevity, and aging-associated diseases has been an active area of research.
Disease management is defined as "a system of coordinated healthcare interventions and communications for populations with conditions in which patient self-care efforts are significant."

Personalized medicine, also referred to as precision medicine, is a medical model that separates people into different groups—with medical decisions, practices, interventions and/or products being tailored to the individual patient based on their predicted response or risk of disease. The terms personalized medicine, precision medicine, stratified medicine and P4 medicine are used interchangeably to describe this concept, though some authors and organizations differentiate between these expressions based on particular nuances. P4 is short for "predictive, preventive, personalized and participatory".
In medicine, patient compliance describes the degree to which a patient correctly follows medical advice. Most commonly, it refers to medication or drug compliance, but it can also apply to other situations such as medical device use, self care, self-directed exercises, or therapy sessions. Both patient and health-care provider affect compliance, and a positive physician-patient relationship is the most important factor in improving compliance. Access to care plays a role in patient adherence, whereby greater wait times to access care contributing to greater absenteeism. The cost of prescription medication also plays a major role.
A chronic condition is a health condition or disease that is persistent or otherwise long-lasting in its effects or a disease that comes with time. The term chronic is often applied when the course of the disease lasts for more than three months. Common chronic diseases include diabetes, functional gastrointestinal disorder, eczema, arthritis, asthma, chronic obstructive pulmonary disease, autoimmune diseases, genetic disorders and some viral diseases such as hepatitis C and acquired immunodeficiency syndrome. An illness which is lifelong because it ends in death is a terminal illness. It is possible and not unexpected for an illness to change in definition from terminal to chronic. Diabetes and HIV for example were once terminal yet are now considered chronic due to the availability of insulin for diabetics and daily drug treatment for individuals with HIV which allow these individuals to live while managing symptoms.
Pharmacotherapy, also known as pharmacological therapy or drug therapy, is defined as medical treatment that utilizes one or more pharmaceutical drugs to improve ongoing symptoms, treat the underlying condition, or act as a prevention for other diseases (prophylaxis).

Self-care has been defined as the process of establishing behaviors to ensure holistic well-being of oneself, to promote health, and actively manage illness when it occurs. Individuals engage in some form of self-care daily with food choices, exercise, sleep, and hygiene. Self-care is not only a solo activity, as the community—a group that supports the person performing self-care—overall plays a role in access to, implementation of, and success of self-care activities.
Race and health refers to how being identified with a specific race influences health. Race is a complex concept that has changed across chronological eras and depends on both self-identification and social recognition. In the study of race and health, scientists organize people in racial categories depending on different factors such as: phenotype, ancestry, social identity, genetic makeup and lived experience. "Race" and ethnicity often remain undifferentiated in health research.
Prescription cascade is the process whereby the side effects of drugs are misdiagnosed as symptoms of another problem, resulting in further prescriptions and further side effects and unanticipated drug interactions, which itself may lead to further symptoms and further misdiagnoses. This is a pharmacological example of a feedback loop. Such cascades can be reversed through deprescribing.
Chronic care management encompasses the oversight and education activities conducted by health care professionals to help patients with chronic diseases and health conditions such as diabetes, high blood pressure, systemic lupus erythematosus, multiple sclerosis, and sleep apnea learn to understand their condition and live successfully with it. This term is equivalent to disease management for chronic conditions. The work involves motivating patients to persist in necessary therapies and interventions and helping them to achieve an ongoing, reasonable quality of life.
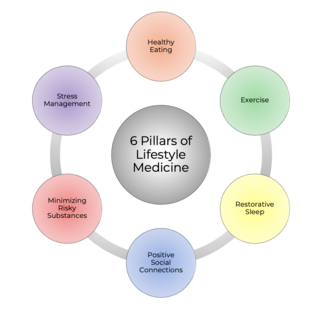
Lifestyle medicine (LM) is a branch of medicine focused on preventive healthcare and self-care dealing with prevention, research, education, and treatment of disorders caused by lifestyle factors and preventable causes of death such as nutrition, physical inactivity, chronic stress, and self-destructive behaviors including the consumption of tobacco products and drug or alcohol abuse. The goal of LM is to improve individuals' health and wellbeing by applying the 6 pillars of lifestyle medicine (nutrition, regular physical activity, restorative sleep, stress management, avoidance of risky substances, and positive social connection) to prevent chronic conditions such as cardiovascular diseases, diabetes, metabolic syndrome and obesity.
The Patient Activation Measure (PAM) is a commercial product which assesses an individual's knowledge, skill, and confidence for managing one's health and healthcare. Individuals who measure high on this assessment typically understand the importance of taking a pro-active role in managing their health and have the skills and confidence to do so.

Diabetes mellitus, often known simply as diabetes, is a group of common endocrine diseases characterized by sustained high blood sugar levels. Diabetes is due to either the pancreas not producing enough insulin, or the cells of the body becoming unresponsive to the hormone's effects. Classic symptoms include thirst, polyuria, weight loss, and blurred vision. If left untreated, the disease can lead to various health complications, including disorders of the cardiovascular system, eye, kidney, and nerves. Diabetes accounts for approximately 4.2 million deaths every year, with an estimated 1.5 million caused by either untreated or poorly treated diabetes.

Finerenone, sold under the brand name Kerendia and Firialta, is a medication used to reduce the risk of kidney function decline, kidney failure, cardiovascular death, non-fatal heart attacks, and hospitalization for heart failure in adults with chronic kidney disease associated with type 2 diabetes. Finerenone is a non-steroidal mineralocorticoid receptor antagonist (MRA). It is taken orally.
Eve Askanas Kerr is an American physician-researcher. Kerr is a Full Professor of internal medicine and the inaugural Vice-Chair of Diversity, Equity, and Well-being at the University of Michigan.
References
- ↑ - Linda Hunt - Professor. Archived 2014-03-10 at the Wayback Machine
- ↑ Hunt, LM; Truesdell, ND; Kreiner, MJ (2013). "Genes, race, and culture in clinical care: racial profiling in the management of chronic illness". Med Anthropol Q. 27 (2): 253–71. doi:10.1111/maq.12026. PMC 4362784 . PMID 23804331.
- ↑ Linda M Hunt - Michigan State University - SciVal Experts 4.6 Archived 2014-04-26 at the Wayback Machine
- ↑ Hunt, Linda M.; Kreiner, Meta J. (2013). "Pharmacogenetics in Primary Care: The Promise of Personalized Medicine and the Reality of Racial Profiling". Culture, Medicine, and Psychiatry. 37 (1): 226–235. doi:10.1007/s11013-012-9303-x. PMC 3593998 . PMID 23264029.
- ↑ "Dr. Linda Hunt Retires from the Department". 23 August 2020.
- ↑ Hunt, Linda M.; Arar, Nedal H. (2008-01-08). "An Analytical Framework for Contrasting Patient and Provider Views of the Process of Chronic Disease Management" . Medical Anthropology Quarterly. 15 (3): 347–367. doi:10.1525/maq.2001.15.3.347. ISSN 0745-5194. PMID 11693036.
- ↑ Bell, Hannah S.; Odumosu, Funmi; Martinez-Hume, Anna C.; Howard, Heather A.; Hunt, Linda M. (2019-04-03). "Racialized Risk in Clinical Care: Clinician Vigilance and Patient Responsibility". Medical Anthropology. 38 (3): 224–238. doi:10.1080/01459740.2018.1476508. ISSN 0145-9740. PMC 6298860 . PMID 29912575.
- ↑ Linda M Hunt - Michigan State University - SciVal Experts 4.6 Archived 2015-12-19 at the Wayback Machine