Related Research Articles

Urology, also known as genitourinary surgery, is the branch of medicine that focuses on surgical and medical diseases of the urinary system and the reproductive organs. Organs under the domain of urology include the kidneys, adrenal glands, ureters, urinary bladder, urethra, and the male reproductive organs.

The prostate is both an accessory gland of the male reproductive system and a muscle-driven mechanical switch between urination and ejaculation. It is found in all male mammals. It differs between species anatomically, chemically, and physiologically. Anatomically, the prostate is found below the bladder, with the urethra passing through it. It is described in gross anatomy as consisting of lobes and in microanatomy by zone. It is surrounded by an elastic, fibromuscular capsule and contains glandular tissue, as well as connective tissue.

Prostate cancer is the uncontrolled growth of cells in the prostate, a gland in the male reproductive system below the bladder. Abnormal growth of prostate tissue is usually detected through screening tests, typically blood tests that check for prostate-specific antigen (PSA) levels. Those with high levels of PSA in their blood are at increased risk for developing prostate cancer. Diagnosis requires a biopsy of the prostate. If cancer is present, the pathologist assigns a Gleason score, and a higher score represents a more dangerous tumor. Medical imaging is performed to look for cancer that has spread outside the prostate. Based on the Gleason score, PSA levels, and imaging results, a cancer case is assigned a stage 1 to 4. A higher stage signifies a more advanced, more dangerous disease.

Benign prostatic hyperplasia (BPH), also called prostate enlargement, is a noncancerous increase in size of the prostate gland. Symptoms may include frequent urination, trouble starting to urinate, weak stream, inability to urinate, or loss of bladder control. Complications can include urinary tract infections, bladder stones, and chronic kidney problems.

Prostate-specific antigen (PSA), also known as gamma-seminoprotein or kallikrein-3 (KLK3), P-30 antigen, is a glycoprotein enzyme encoded in humans by the KLK3 gene. PSA is a member of the kallikrein-related peptidase family and is secreted by the epithelial cells of the prostate gland in men and the paraurethral glands in women.

Prostate biopsy is a procedure in which small hollow needle-core samples are removed from a man's prostate gland to be examined for the presence of prostate cancer. It is typically performed when the result from a PSA blood test is high. It may also be considered advisable after a digital rectal exam (DRE) finds possible abnormality. PSA screening is controversial as PSA may become elevated due to non-cancerous conditions such as benign prostatic hyperplasia (BPH), by infection, or by manipulation of the prostate during surgery or catheterization. Additionally many prostate cancers detected by screening develop so slowly that they would not cause problems during a man's lifetime, making the complications due to treatment unnecessary.
Prostate cancer screening is the screening process used to detect undiagnosed prostate cancer in men without signs or symptoms. When abnormal prostate tissue or cancer is found early, it may be easier to treat and cure, but it is unclear if early detection reduces mortality rates.

High-intensity focused ultrasound (HIFU), or MR-guided Focused Ultrasound Surgery is an incision-less therapeutic technique that uses non-ionizing ultrasonic waves to heat or ablate tissue. HIFU can be used to increase the flow of blood or lymph or to destroy tissue, such as tumors, via thermal and mechanical mechanisms. Given the prevalence and relatively low cost of ultrasound generation mechanisms, the premise of HIFU is that it is expected to be a non-invasive and low-cost therapy that can at least outperform care in the operating room.

Cryoablation is a process that uses extreme cold to destroy tissue. Cryoablation is performed using hollow needles (cryoprobes) through which cooled, thermally conductive fluids are circulated. Cryoprobes are positioned adjacent to the target in such a way that the freezing process will destroy the diseased tissue. Once the probes are in place, the attached cryogenic freezing unit removes heat from ("cools") the tip of the probe and by extension from the surrounding tissues.
Urology Robotics, or URobotics, is a new interdisciplinary field for the application of robots in urology and for the development of such systems and novel technologies in this clinical discipline. Urology is among the medical fields with the highest rate of technology advances, which for several years has included the use medical robots.
Treatment for prostate cancer may involve active surveillance, surgery, radiation therapy – including brachytherapy and external-beam radiation therapy, proton therapy, high-intensity focused ultrasound (HIFU), cryosurgery, hormonal therapy, chemotherapy, or some combination. Treatments also extend to survivorship based interventions. These interventions are focused on five domains including: physical symptoms, psychological symptoms, surveillance, health promotion and care coordination. However, a published review has found only high levels of evidence for interventions that target physical and psychological symptom management and health promotion, with no reviews of interventions for either care coordination or surveillance. The favored treatment option depends on the stage of the disease, the Gleason score, and the PSA level. Other important factors include the man's age, his general health, and his feelings about potential treatments and their possible side-effects. Because all treatments can have significant side-effects, such as erectile dysfunction and urinary incontinence, treatment discussions often focus on balancing the goals of therapy with the risks of lifestyle alterations.

Roger Sinclair Kirby FRCS(Urol), FEBU is a British retired prostate surgeon and professor of urology, researcher, writer on men's health and prostate disease, founding editor of the journal Prostate Cancer and Prostatic Diseases and Trends in Urology and Men's Health and a fundraiser for prostate disease charities, best known for his use of the da Vinci surgical robot for laparoscopic prostatectomy in the treatment of prostate cancer. He is a co-founder and president of the charity The Urology Foundation (TUF), vice-president of the charity Prostate Cancer UK, trustee of the King Edward VII's Hospital and as of 2020 is president of the Royal Society of Medicine (RSM), London.
Specimen provenance complications (SPCs) result from instances of biopsy specimen transposition, extraneous/foreign cell contamination or misidentification of cells used in clinical or anatomical pathology. If left undetected, SPCs can lead to serious diagnostic mistakes and adverse patient outcomes.
DNA Specimen Provenance Assignment (DSPA) also known as DNA Specimen ProvenanceAssay, is a molecular diagnostic test used to definitively assign biopsy specimen identity and establish specimen purity during the diagnostic testing cycle for cancer and other histopathological conditions. The term first appeared in the 2011 scientific paper, “The Changing Spectrum of DNA-Based Specimen Provenance Testing in Surgical Pathology,” published in the American Journal of Clinical Pathology, which built upon concepts described in an earlier paper published in the Journal of Urology.

Prokar Dasgupta is an Indian-born British surgeon and academic who is professor of surgery at the surgical academy at King's Health Partners, London, UK. Since 2002, he has been consultant urologist to Guy's Hospital, and in 2009 became the first professor of robotic surgery and urology at King's, and subsequently the chairman of the King's College-Vattikuti Institute of Robotic Surgery.
PI-RADS is an acronym for Prostate Imaging Reporting and Data System, defining standards of high-quality clinical service for multi-parametric magnetic resonance imaging (mpMRI), including image creation and reporting.
Caroline M. Moore is the first woman to be made a professor of urology in the United Kingdom. She works in the diagnosis and treatment of prostate cancer at University College London.

The Urology Foundation (TUF) is a charity that works across the UK and Ireland with the aim of improving the knowledge and skills of surgeons who operate on diseases of the male and female urinary-tract system and the male reproductive organs and funds research to improve outcomes of all urological conditions and urological cancers.
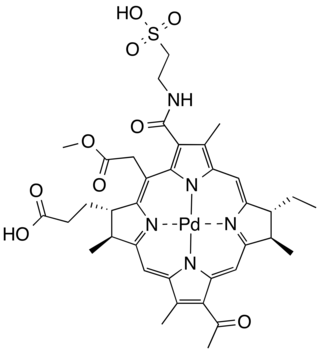
Padeliporfin, sold under the brand name Tookad, is a medication used to treat men with prostate cancer. It is used in the form padeliporfin di-potassium.
Mark Emberton is a urologist and prostate cancer research specialist using novel imaging techniques and minimally invasive treatments to improve diagnosis and treatment of prostate cancer.
References
- 1 2 NHS:Professor Hashim U. Ahmed
- 1 2 3 Imperial College healthcare: Professor Hashim U. Ahmed
- 1 2 Cromwell Hospital:Professor Hashim Ahmed, Consultant Urological Surgeon
- ↑ List of Registered Medical Practitioners: Dr. Hashim Ahmed
- ↑ Ahmed, H. U. (2014-02-28). An evaluation of focal therapy in the treatment of localised prostate cancer (Doctoral thesis). UCL (University College London).
- 1 2 Prostate Cancer UK: Spotlight on: Professor Hash Ahmed
- ↑ Imperial College London: New steam treatment offers hope for men with an enlarged prostate
- ↑ The Telegraph: Five-minute steam treatment that shrinks enlarged prostate offers hope for millions of men
- ↑ Prostate cancer uk:Focusing on targeted treatments to reduce side effects
- ↑ Cancer Therapy Advisor: Men With Prostate Cancer Willing to Accept Worse Survival Odds to Improve QoL
- ↑ The Telegraph: Prostate cancer could be ruled out with simple MRI scan which prevents 25,000 biopsies
- ↑ "NHS England: Implementing a timed prostate cancer diagnostic pathway" (PDF). Archived from the original (PDF) on 2021-01-20. Retrieved 2020-02-08.
- ↑ The Guardian: MRI twice as likely as biopsy to spot prostate cancer, research shows
- ↑ NHS: RAPID diagnostic prostate cancer pathway
- ↑ "NHC RM Partners: Professor Hashim Ahmed on the RAPID prostate diagnostic pathway". Archived from the original on 2021-06-07. Retrieved 2020-02-08.
- ↑ Prostate Cancer UK: How playing the long game and your donations led to mpMRI breakthrough
- ↑ BBC News: MRI scanning for prostate cancer biggest advance 'in decades'
- ↑ National institute for health research: Magnetic Thermoablation in the Treatment of Early Prostate Cancer
- ↑ NIHR: A randomised controlled trial of Partial prostate Ablation versus Radical prosTatectomy (PART) in intermediate risk unilateral clinically localised prostate cancer a feasibility study
- ↑ NIHR: A randomised controlled trial of Partial prostate Ablation versus Radical Treatment (PART) in intermediate risk, unilateral clinically localised prostate cancer
- ↑ Grand Rounds in Uroiogy: Dr. Hashim U. Ahmed on Today’s Focal Therapy For Prostate Cancer